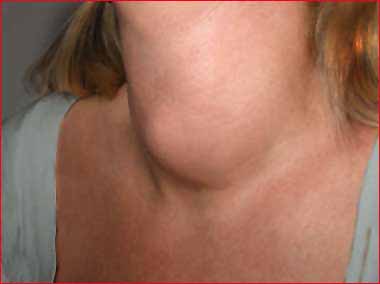
Goiter Treatment
Goiter, also referred to as bronchocele, is a condition that is manifested by the significant thyroid gland swelling. The condition is also associated with neck or laryngeal swelling. It has been reported that women are at a higher risk of developing goiter. Some of the common symptoms of goiter include breathing difficulty, persistent cough, and dysphagia due to increased size of thyroid gland. The treatment for goiter mainly aims at relieving symptoms like general malaise. A holistic approach that includes lifestyle modifications can effectively help to manage goiter. Here is a detailed outline about the treatment protocol for goiter that discusses about various treatment modalities, surgical treatment, and management of the condition.
Medication therapy
Initially, an endocrinologist should frequently examine the patient in case of goiter that is associated with malignancy or thyroid dysfunction or if the case requires surgical management.
No treatment is required for small and benign euthyroid goiters as the efficacy of medical treatment with thyroid hormone is still a matter of debate. A combination of medical and surgical treatment is recommended for malignant goiters; large and complicated goiters. Levothyroxine suppressive therapy helps to reduce the size of benign euthyroid goiter. Frequent monitoring is necessary to ensure low serum TSH levels to avoid cardiac arrhythmia, hyperthyroidism, and osteoporosis during the treatment course. Suppressive treatment is also recommended for Hashimoto thyroiditis. Some doctors advice suppressive therapy for a definite period of time rather than indefinite therapy.
The treatment that is reinforced for treating hypothyroidism or hyperthyroidism type of goiter works by reducing the size of thyroid gland. Endemic goiter can be treated with levothyroxine or iodine supplementation to reduce the size of goiter. Levothyroxine and anti-inflammatory medication is used to treat goiters with autoimmune thyroiditis. Levothyroxine is also effective in treating congenital goiters. Benign thyroid nodules can be effectively treated with ethanol infusion.
Thyroid hormone replacement therapy
Thyroid hormone replacement therapy is advised for goiter patients who have been treated with a combination of surgical and radiation treatment. L-thyroxine thyroid hormone medication is effective in treating hypothyroidism. This is because, it causes partial shrinkage of the gland in case of enlarged and under active thyroid with high TSH level caused by autoimmune or Hashimoto thyroiditis. Thyroid hormone therapy is also suggested for benign goiters. Levothyroxine sodium is the most commonly prescribed thyroid hormone that should be taken daily. Frequent administration of Liothyronine sodium is also helpful. Liotrix, thyroglobulin, and Dessicated thyroid powder are also suggested.
Radioactive iodine therapy
Treatment with radioactive iodine reduces the size and controls the over-activity of the thyroid gland. Radioactive iodine is the preferred treatment of choice to treat toxic nodular goiter, hyperthyroid goiter caused by Graves’ disease. Treatment of nontoxic goiter with radioactive iodine is still not desirable. However, radioactive iodine therapy effectively shrinks some types of nontoxic nodular goiters associated with normal function. Radioactive iodine is usually indicated for treating goiter or nodule associated with an overactive thyroid gland. Sometimes, it is also used to reduce not so overactive goiters.
Surgical Treatment
Surgical excision of the thyroid gland (thyroidectomy) is required in case of severely enlarged thyroid gland often leading to the compression of adjacent structures, including blood vessels. Thyroid nodules are also treated with combination therapy, including radioactive iodine and surgery depending on the level of thyroid over-activity and its size. Thyroid nodules, suggestive of malignancy should be completely removed along with large portion of thyroid gland to avoid the invasion of thyroid cancer to other parts of the body. Many cases with no apparent evidence of malignancy may also require surgical excision of the nodule and at least 50 percent of thyroid gland. This is due to a fact that 1 in 7 patients presenting with nodules tend to develop thyroid cancer. However, it has been relatively ineffective by treating these patients with thyroid hormone to shrink thyroid nodules.
Surgery is indicated for the following thyroid conditions:
When other treatment modalities prove to be ineffective or impractical
Malignancy
Large goiters that compress the underlying structures and vessels
Before surgery, the patient condition should be preoperatively treated to achieve a euthyroid state. Maintenance of stabilized airways is crucial. Hemodynamic monitoring is imperative preoperatively in case of hyperthyroidism or hypothyroidism. Emergency surgical treatment of hypothyroid goiter requires intravenous gluco corticoids and levothyroxine at recommended doses. Emergency surgical treatment of thyrotoxic goiter requires beta-blockers, prescription anti-thyroid drugs, and glucocorticoids. Suppressive iodine doses can also work. Postoperative therapy requires serum calcium level monitoring. Post-operatively, Goiters with primary thyroid malignancy require radioactive iodine ablation and levothyroxine replacement therapy. Primary malignancy should be treated in case of metastatic lesions of thyroid gland.
>>> Regaining your Emotional and Physical Health <<<
Diet modification
Endemic goiter can be concurrently influenced by various nutritional factors such as protein malnutrition, deficient intake of dietary iodine, energy malnutrition, and intake of goitrogens.
Endemic goiter can be treated with dietary Iodine supplementation and by avoiding the intake of goitrogens.
Goitrogen containing foods prevent the iodide uptake of thyroid gland, which include bamboo shoots, cassava, sweet potatoes, lima beans, maize, and vegetables that belong to the Cruciferae family.
Filed Under: Goiter Treatment